FAQs
NOTE: it is important for everyone to know the facts and fiction when applied to concussion!
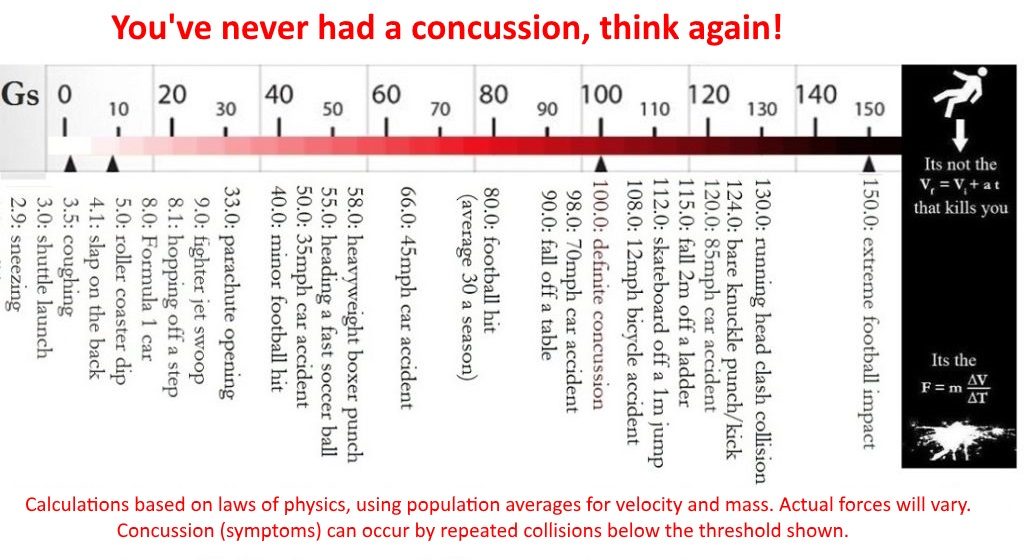
The chart below demonstrates how easily you can get a concussion, and major sports have conditioned us not to question headaches and dizziness from minor collisions.
No blood, no problems, yes you do have a concussion!
What is a concussion?
Consistent headaches.
Ringing in ears.
Dizziness.
Vision problems.
Not thinking clearly.
Trouble remembering new information.
Sensitivity to light.
Sensitivity to noise.
Sluggishness.
Behavior or personality changes.
Concentration difficulties.
Feeling sad, nervous, or easily angered.
Sleeping more or less than usual.
Anxiety.
Depression.
Would a doctor ignore concussion symptoms?
A Doctor’s first question is either “how are you”, “how can I help you”, “what seems to be the problem” or “what happened to bring you here”? Which is all part of a Doctor understanding the circumstances to make a diagnosis.
Conditions that share symptoms with concussion get a lot of media coverage. Most have medications that are easily available and heavily marketed to the medical community.
YOU must tell the doctor that you have had a previous head injury or the doctor will recall the possible outcomes from the causes they are mindful of, such as:
ADHD
ADD
Autism
PTSD
Mold reaction
chronic fatigue syndrome (CFS)
fibromyalgia syndrome (FMS)
Anxiety
Depression
Shared Symptoms
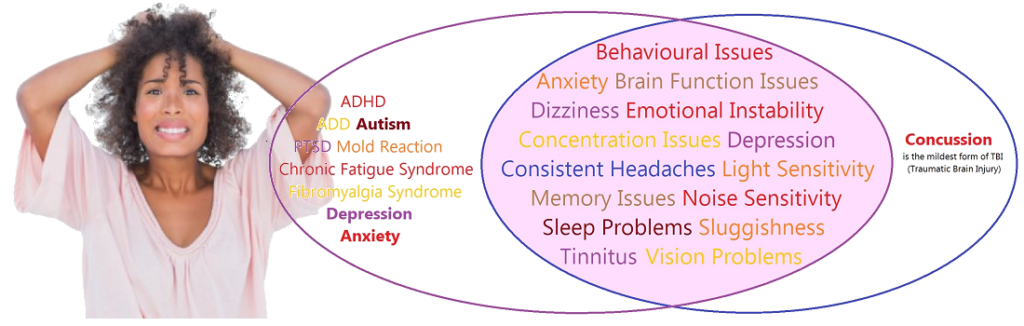
Unless you tell the doctor that you have had a previous head injury, they will not usually be considering concussion as a possible cause of symptoms that are shared with high profile conditions such as Depression, Anxiety, PTSD and Autism.
Worse when you have a 10 minute appointment and reel of 5 or more symptoms. The Doctor is trying to listen and think at the same time.
If the patient is unaware themselves that they had suffered a concussion. The Doctor can’t be criticised for missing the diagnosis.
Everyone knows a child or adult who has problems:
Not thinking clearly.
Trouble remembering new information.
Consistent headaches.
Vision problems.
Dizziness.
Sensitivity to light.
Sensitivity to noise.
Sluggishness.
Ringing in ears.
Behavior or personality changes.
Concentration difficulties.
Feeling sad, nervous, or easily angered.
Sleeping more or less than usual.
Anxiety.
Depression.
These are ALL concussion symptoms, some years old, even from a childhood injury.
These symptoms can and do get attributed to other conditions such as:
Depression
Anxiety
Autism
PTSD
ADHD
ADD
Mold reaction
chronic fatigue syndrome (CFS)
fibromyalgia syndrome (FMS)
The result can be unnecessary treatment, medication, loss of self esteem, social isolation and a child or adult will quickly drop behind their peers.
Why don’t I remember my concussion?
In most cases the patient or their family won’t recall the actual head injury, or no-one other than the patient will be aware of the incident.
Common symptoms of concussion:
Temporary loss of consciousness
Amnesia surrounding the traumatic event
Headache or a feeling of pressure in the head
Confusion or feeling as if in a fog
Dizziness or “seeing stars”
Ringing in the ears
Nausea
Unless these symptoms make the patient very weak and infirm or there are external signs of an injury (bleeding etc) requiring medical assistance, the symptoms thus the chance of a concussion are mostly ignored.
Why can’t I train or play sport for several weeks when I have a concussion?
You CAN exercise but not in a way that puts you at risk of a further head injury UNTIL you are fully recovered.
“Recovery” from a concussion may be just the more extreme symptoms abating, therefore you may believe a return to a normal state of health has occurred.
If you suffer another head knock whilst recovering from a previous concussion you can set back your recovery, and leave residual symptoms that can last the rest of your life!
Worse is Second Impact Syndrome, if a player returns to the game or practice too early, and there is severe brain swelling a further concussive event can be FATAL!
Can I sleep with a concussion?
If a concussion is suspected a medical professional should be consulted.
Due to other possible symptoms, such as vomiting and loss of consciousness the concussed person should not be left alone the first night.
Current research shows that sleeping is good for a concussed person. Getting physical and mental rest helps recovery from a concussion.
If any symptoms are ongoing a medical professional should be consulted.
Why can’t I self assess if I have a concussion?
Concussion symptoms:
Headache or a feeling of pressure in the head.
Temporary loss of consciousness.
Confusion or feeling as if in a fog.
Amnesia surrounding the traumatic event.
Dizziness or “seeing stars”
Ringing in the ears.
Nausea.
Vomiting
Usually take away basic decision making capabilities. Which is why the patient should NOT be person assessing the injury!
What does a full recovery from concussion mean?
There is a common consensus from Researchers and Doctors that the only true measure that a full recovery from concussion has occurred, is a return to pre-injury behaviour.
The measure for this is extremely difficult if no baseline has been set for the individual.
Why use a phone app?
If you knew that recording all head injuries could help your child’s future mental health – would you do it?
Concussions share symptoms with many other conditions.
The most difficult elements to diagnose concussion is that symptoms may not become apparent for a number of years.
Concussions can be cumulative!
When there was no blood or visual bump, it may seem okay, however after a time symptoms may become apparent.
Would you remember the original incident?
Could you tell the doctor?

Has your child been highlighted as having attention problems or inability to sit still?
We need to start recording any and every head injury in a central database that can be kept and updated for life.
Minder Foundation are establishing FREE online baseline, post-concussion and rehabilitation tests.
Plus provide a FREE online user panel and easy to use phone app to do the tests or upload details of ANY head injuries.
These will allow patients, parents and Medical Professionals to maintain historical data and monitor changes thru a head injury.
The resultant database will also provide a valuable (free) source of anonymous data for all bonafide researchers.
What is a baseline test?
A baseline neurocognitive exam measures a person’s cognitive function (e.g. ability to think), generating a score to serve as a reference point (a “baseline”) against which to compare scores on tests performed after the same person sustains a head injury.
The results of the baseline are also helpful in identifying pre-existing conditions that may affect post-injury test results, that have little or nothing to do with head trauma, such as migraine headaches, attention deficit disorder (ADD), attention deficit hyperactivity disorder (ADHD), depression, anxiety disorders, and panic attacks, all of which can significantly skew test results, and have recently prompted calls for the development of separate normative data for athletes with learning disabilities (LD), ADHD, and LD/ADHD diagnosis on computerized neurocognitive test batteries.
Some states and organisations are currently doing baseline tests in an ad hoc manner, mainly with athletes involved in selected sports and at a cost.
Experts also state that more than one type of test is necessary to compile a comprehensive baseline.
Minder Foundation take this one step further, by collating the best of these tests, and configuring the test so that it is available via a FREE phone app and your own personal online panel, EVERYONE will be able to establish a baseline for themselves.
Then given that you have a head injury, you can then be re-tested against your baseline to assist in determining the residual effects of your injury!
Minder Foundation needs your help toward the cost of developing the full test, and providing the database on which each individual can maintain their records.
Why won’t a helmet stop concussion?
A helmet can lessen blunt trauma injuries (fractures/cuts/abrasions) but cannot extend the time (by providing a sufficient cushion effect) of acceleration/deceleration sufficiently to stop concussions.
In layman’s terms, if your head stops quickly, as in hitting the ground, the force is HUGE = concussion.
This can happen in a fall, where the head hits the floor and the brain stops (decelerates) immediately or worse, bounces so it goes thru rapid deceleration, then acceleration in the opposite direction!
Your head can also be thrown violently when your body gets hit, such as in a football tackle, or a car accident. Other injuries such as neck/spinal usually occur and are more obvious, in a lot of cases the concussion isn’t even addressed.
Impacts where the head gets torsional (rotation) forces so the skull and the brain are forced to spin can cause the most severe symptoms.
Why do girls get more concussions than boys?
Research is not conclusive, but our observations are that boys play rougher than girls as small children. This allows them to build spacial awareness whilst they are learning their physical capabilities.
Older children are bigger, stronger, faster and usually more competitive/aggressive. Thus more capable of injuring themselves, which is when girls are developing their spacial awareness in sports games.
Why are there more concussions in non-contact sports than contact sports?
Again the research is inconclusive, but our observations are that most non-contact sports involve running in a head down attitude, looking down at the ball. This causes players heads to be the first point of contact.
In contact sports the players run more heads up, and are expecting and readying themselves to be tackled, thus more prepared for impact.
Why is the Zackery Lystedt Law so important?
The enactment of this law in Washington State was the first legal recognition of the importance of protecting sportspeople from over-enthusiasm by coaches, parents or the athletes themselves.
Returning to play has had life altering consequences for Zack, the subsequent realisation that consequences of concussions can be mitigated, has caused several states and even other countries to look at this law as a protective mechanism.
The basic premise of the law is that any player who is thought to have suffered a head injury, must be evaluated and cleared by a medical professional prior to returning to play.
The Zach Lysted Law and similar are being enacted to stop obviously concussed players from being put back in play, but current practices still allow concussed players that aren’t obviously hurt to continue playing.
Will supporting this project hurt my favorite sport?
The opposite should apply, as education brings subtle changes to how sports are played. Such as the NFL “Heads Up” campaign.
With measurement devices becoming more sophisticated, cheaper and more widely used. Better and more complete data will speed up the transition to knowing as against hypothesis currently employed.
Sports will be able to foresee and mitigate injuries that currently create hostile reports, adverse public perception, high medical, social and insurance costs.
Parents will again be comfortable in their children supporting and participating in sports that are currently seen as potentially harmful.
TBI or ABI?
While similar, there is a distinction between the two types of brain injuries. TBIs (Traumatic Brain Injuries) are injuries to the brain caused by an external force. ABIs (Acquired Brain Injuries) are a broader category of brain injuries; they include injuries to the brain as a result of stroke or other illness that affects the brain. Although many people use the terms interchangeably, TBIs are actually a subcategory of ABIs.
Footnote, Concussion the movie:
The human skull is not designed for heavy impact.
As correctly stated in ‘Concussion‘, “the Cape Gannet, Red Hooded Woodpecker and Big Horn Sheep have a mechanism that allows massive deceleration of the skull to not affect the brain.
Humans don’t have this facility, the human brain has the consistency of jello, being comprised primarily of cell bodies (grey matter) and axons (white matter) which are of significantly different densities. Any rapid acceleration transmitted to the impacted skull, both linear and rotational, will almost certainly cause shearing between the 2 dissimilar materials. This occurs primarily in the Axons, and the damage cannot be detected by scans unless bleeding is present. Scientists insist the only way of telling conclusively if a person is still suffering a concussion is if their behaviour has returned to normal!
What can I do?
Until our online facility is functional you need to keep a record of any head injuries your family has. When you visit a doctor with a related symptom or new injury recount to the doctor the patient’s head injury history.
Minder Foundation are establishing FREE online baseline, post-concussion and rehabilitation tests.
Plus provide a FREE online user panel and easy to use phone app to do the tests or upload details of ANY head injuries.
These will allow patients, parents and Medical Professionals to maintain historical data and monitor changes thru a head injury.
The resultant database will also provide a valuable (free) source of anonymous data for all bonafide researchers.
Have you seen someone suffering and wondered what YOU can do?
Be a Head Injury Hero and help us continue to provide these services by donating now.
Statements on this page are based on research, ours and others, and should not be used in assessing a TBI, (contact a medical professional), links to research can be found here…
#humptychallenge #430million #minder #minderfoundation #concussion #headinjuryhero #headinjury @humptychallenge
